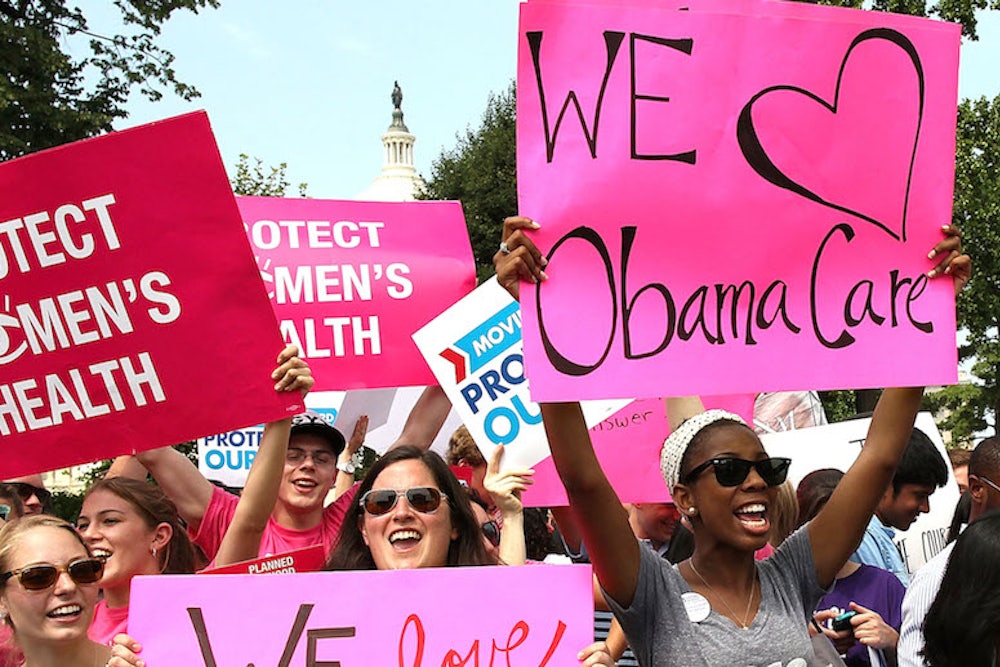Federal judges issue conflicting ruling about Obamacare. The law’s supporters predict, confidently, that they will eventually prevail. The people who need health insurance watch to see whether the courts will take it away.
Yes, we’ve seen this play out before. It happened a few years ago, when critics of the Affordable Care Act challenged the constitutionality of its individual mandate. And just like that effort, this one will probably fail, although the outcome is far from certain.
But for all the parallels, there’s one crucial difference.
The previous lawsuits were about some big, weighty issues—namely, the boundaries of federal power and the extent of personal freedom. The plaintiffs, whatever their true motives, at least claimed to be fighting on behalf of liberty.
These new lawsuits, about which two courts issued conflicting rulings on Tuesday, make no similarly lofty claims of principle. They focus, instead, on some ambiguous text in the language of the law and allegation that Congress intended the law to work differently than the Obama Administration says.
Oh, the legal briefs make some real arguments about constitutional principles and it's entirely possible that the plaintiffs who wrote those briefs believe them. But it’s hard to escape the conclusion that these arguments are altogether secondary to the real goal here—that these lawsuits are simply one more attempt to cripple Obamacare and yank insurance away from millions of people, no matter what it takes.
Think back to the issues that were at stake in NFIB v. Sebelius, the case against the mandate that eventually made its way to the Supreme Court. The mandate is a requirement that people buy insurance, if it’s affordable, or pay a fine. Critics said the mandate amounted to coercion. Making people get insurance, the argument went, was like making people buy broccoli. It might be good for you, the argument went, but the federal government had no power to make individuals do it. In response, the Obama Administration and the law's defenders responded by saying the mandate fell within congressional authority to “regulate commerce” and to levy taxes, at least as the courts had defined those powers for decades. The commerce argument didn't prevail at the Supreme Court but the tax argument did—and the law (mostly) survived.
These new lawsuits focus on a different aspect of the law: the tax credits, worth thousands of dollars a year in some cases, for people who buy insurance through Obamacare's new marketplaces. Under the Affordable Care Act, states have a choice. They can set up and operate their own marketplaces. Or they can ask the Department of Health and Human Services (HHS) to take on that task. It turns out that the section of the law authorizing the federal government to dispense those tax credits mentions the state-run marketplaces, but not the ones that HHS manages. And therein lies the problem.
According to the lawsuits, which are the brainchild of Michael Cannon from the Cato Institute and Jonathan Adler from Case Western University, the ambiguity is no accident. Obamacare’s architects intended to use the subsidies as incentive for states to manage their own marketplaces. (Cannon and Adler weren't the only ones making this case, but, as my colleague Alec MacGillis has written, Cannon in particular is the person most responsible for crafting and spreading this argument.)
As many experts (and I) have written before, the theory is inconsistent with the rest of the statute, the discussions of the law prior to passage, and what the people who wrote the statute say now. An amicus brief from the law's sponsors attests to the fact that they never intended to deny anybody subsidies just because states asked HHS to handle the work of regulating its insurance policies. Also among those who think the Cannon-Adler theory is nonsense is Liz Fowler, who as chief health care counsel on the Senate Finance Committee during the law's crafting probably understood congressional intent better than anybody. “Of course Congress did not intend to deny anyone in any state access to tax credits to which they are entitled,” she has said.
That argument prevailed in two lower federal courts that considered the cases previously. And it prevailed again on Tuesday, in the Fourth Circuit Court of Appeals, when a three-judge panel ruled unanimously that the subsides are ok. But a three-judge panel from the D.C. Circuit, also ruling on Tuesday, split along partisan lines. The two Republican appointees ruled in favor the lawsuits.
For now, nothing changes. The Obama Administration has sought an “en banc” appeal, which means it’s seeking a ruling from all of the active judges on the D.C. Circuit. Democratic appointees are a clear majority there, so most legal experts think the administration will prevail. (For a legal argument against the ruling, see Ian Millhiser's analysis.) Meanwhile, two more cases are working their way up through the courts. Eventually the issue may come before the Supreme Court, although it’s not a given. If the en banc ruling goes the Administration's way and no other courts rule in favor of the lawsuits, the justices could simply pass on the case altogether—allowing the law to stand and to operate as it does now.
As with the mandate lawsuits, the stakes here are enormous. California, Kentucky, and 14 other states plus the District of Columbia opted to create and run their own exchanges. All the other states, including behemoths Florida and Texas, decided to let HHS handle the job. According to an estimate by researchers at the Urban Institute and funded by the Robert Wood Johnson Foundation, about 11.7 million people in those states will be getting insurance through the marketplaces by 2016, the year such a case would likely come before the Supreme Court. Of those, about 7.3 million would be receiving subsidies.
If somehow the case made it to the Supreme Court and the lawsuit prevailed there, those 7.3 million people would stop receiving federal money. Without that assistance, they'd suddenly have to pay hundreds, even thousands of dollars more for their insurance. (The average premium increase, according to an Avalere Institute study that my colleague Danny Vinik has cited, would be 75 percent.) Many of these people would stop getting insurance altogether.
That wouldn’t be the end of the story. Most likely, HHS would find some way for state officials to “take over” ownership of the marketplaces, even if it meant effectively contracting out much of the management right back to HHS. But those state officials would still have to take some kind of action. Some might not, at least right away.
One plausible scenario is that a familiar political disparity emerges. States like Arizona, Michigan, and Ohio—where Republican officials have already found a way to embrace the law’s Medicaid expansion, in spite of opposition from fellow Republicans—would agree to the new arrangement or start running the exchanges on their own. It’d be an even better deal for their states than the Medicaid expansion, since the federal government picks up the entire cost of subsidies. And, as Brian Beutler notes, they’d be under enormous pressure—from insurers, hospitals, and most important, consumers—to take the money on which so many people already relied.
But in more clearly conservative states that have held out on Medicaid—including behemoths Florida and Texas—the tax credits might really disappear. Just like that, millions would see their premiums jump and/or lose insurance altogether. And the effects could extend to the other parts of the law, for reasons Larry Levitt, senior vice president at the Kaiser Family Foundation, explained well over e-mail:
While the decision directly affects only the subsidies in states not running their own exchanges, it’s not clear the individual market as a whole could function in those states under these circumstances. Without subsidies and a weakened individual mandate—because so many people would be exempt since coverage would now be unaffordable—the risk pool would be skewed towards sicker people. Premiums would rise and insurers would likely exit the market.
In other words, it's not just the subsides that might go away if the lawsuits prevail and states don't opt to run their own exchanges. The law's other popular features—like the availability of decent coverage to all people, regardless of pre-existing condition—would be in danger, at least in those states were conservatives were most opposed to the law. The red-blue divide, already a fact of life in health care, would get even deeper.
And for what? Nobody, not even the plaintiffs in these suits, claim that there’s something fundamentally unjust about having government help people pay for their insurance. The government subsidizes all kinds of activities, from home-buying to paying for college. Conservatives may not like these programs on policy grounds, but you don't hear them claiming it violates anybody's freedom.
At best, this is a case about how literally courts should interpret the text of a statute and how much they should defer to executive agencies in cases of ambiguity—real issues, to be sure, but ones about which nobody said a peep until long after Obamacare became law.
And at worst? It’s an attempt to exploit a drafting error, the kind that happens all the time with complex legislation, in order to get one last shot at repealing a program that has already helped millions to get insurance but that drives libertarians and conservatives crazy. As Dave Weigel notes at Slate, critics like Cannon have made no secret of their desire to stop the law "by any means necessary."
Their attempt probably won’t succeed. But "probably" still isn't "definitely." It's still hard to believe.