This article was originally published on SyriaDeeply.com. To sign-up for SyriaDeeply's daily newsletter, visit SyriaDeeply.com.
Last week, New York Times columnist Nick Kristof nominated Syria as the world capital of human suffering. It’s not just the direct consequences of war: the bombs, rockets, artillery, bullets and now gas rained down upon the civilian population. The Assad regime is also deliberately targeting the people, facilities and services that previously delivered health care to the citizens of Syria, and which, if restored, could even now considerably reduce that suffering.
War is obviously horrible for your health. Collateral damage (the unintentional “side effects” of conflict on civilians when war is conducted according to the rules) is bad enough, but how do you capture what happens when civilians are the object of attack, hospitals are intentionally destroyed, breadlines are deliberately bombed, doctors are targeted for detention and torture, schools are set on fire, and public health systems are shut down?
Last month, I went to Lebanon to launch a population-level study of the long-term impact of the abuses in Syria on civilian health; in other words, to measure some of this suffering, to demonstrate not just the direct effects on health at the moment of an abuse, but the longitudinal effects of sustained denial of medical care. I talked with the haves and the have-nots, the registered and the unregistered, Syrians and Palestinians, Christians and Muslims, fighters, rebels and civilians of all kinds.
They told me about violations of medical neutrality at every level – naming the hospitals, clinics and pharmacies destroyed, the clearly marked ambulances gunned down, the paramedics shot, the pharmacists and doctors tortured to death. And they told me about the impact on themselves and their families.
I saw children with asthma and allergies without their inhalers or epipens. Teenagers with epilepsy without their anticonvulsants. A 10-year-old with cerebral palsy but without his wheelchair or glasses, left behind in Raqqa when the shelling started and his mother had to pick him up and run for their lives. People living with tuberous sclerosis and schizophrenia, heart disease and hypertension without access to either medication or the specialists that used to look after them.
Too many stories from mothers who “miscarried” at five, six or seven months after missile attacks; others whose babies were stillborn at eight months or at term, or died after a few days or months. I played with smiling babies too – but also those with pertussis and pneumonia, giardiasis and rickets, unvaccinated and unprotected.
The widespread evidence of physical trauma is particularly striking: the injuries and amputations, the disabilities and disfigurements, hemiplegias and handicaps sustained by both children and adults. I saw men and children with paralyzed, useless hands, no longer able to write their name. Harmed and humiliated men who had lost not only their bodily functions, but also their livelihoods, their ability to provide and protect their families.
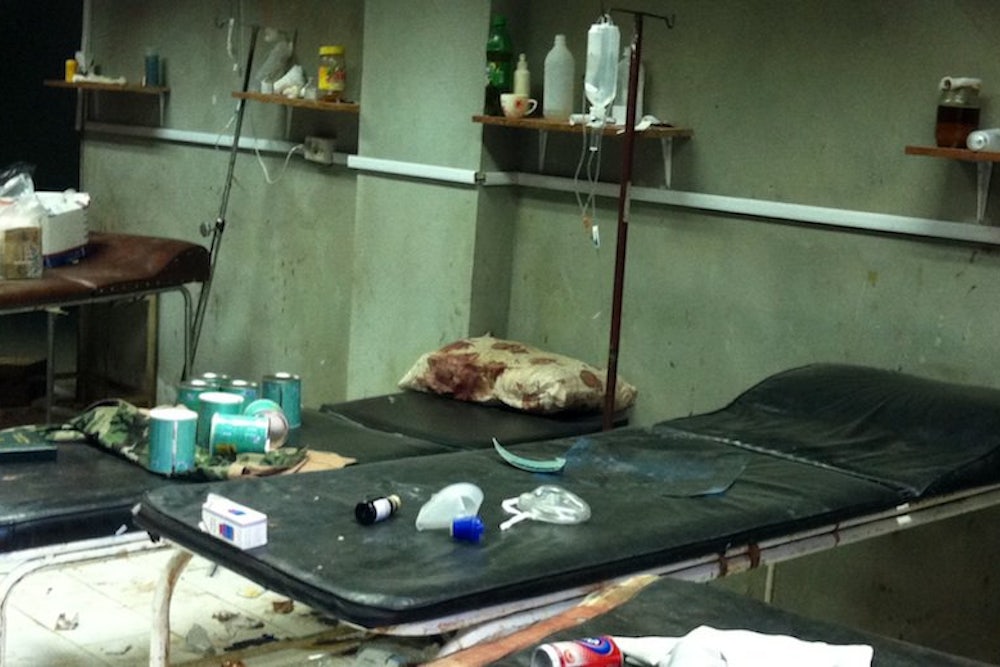
The “field hospitals” that are often the only medical option in rebel-held territory are nothing like a hospital, but much more like a field. A tent between farms, a room in a basement, staffed not by orthopedic, plastic and neurosurgeons but by internists and nurses who can only stem the hemorrhage, stitch up the wounds and save the life of those injured, whether the patient is a 10-year-old girl with a severed arm from a missile during Eid, a rebel fighter or a relief worker trying to evacuate families. There is no option or surgical expertise for more complex nerve reattachment, muscle repair or tendon transfer, let alone fixation of fractures or reconstructive surgery.
A spinal injury shouldn’t necessarily mean hemiplegia, a head injury shouldn’t have to result in loss of vision, yet imaging to see where the shrapnel is lodged, let alone the medical capacity to restore function or undertake reconstructive surgery, is pretty much available only for those who are allowed to enter government-controlled hospitals. No pain medication is awful, and so is no antibiotics, because war wounds become infected easily, which can result in gangrene or septicemia.
The Syrian military also target the field hospitals. For many sick and injured I interviewed, it was too dangerous even to attempt to reach these clinics. One mother has a 15-year-old in Damascus who lost half his face to a shell, but he is unable to travel to Beirut for medical care because vans carrying the injured to Lebanon are targeted too. Another man told me about being targeted as he and 22 others were travelling to Beirut for the surgeries they needed that were unavailable in Syria.
“I got out of the microvan for 2 minutes, for a cigarette … and watched a missile hit the van. All my friends were turned into dust.”
Beyond physical injuries, I was struck by the rise of infectious diseases that are more reminiscent of 19th century Britain. In both places, the rapid urbanization, overcrowded living conditions, lack of sanitation and waste disposal (no toilets or trash collection), the use of child labor and food insecurity led to a radical increase in infectious disease and infant mortality. And yet in Syria we are seeing not only the usual suspects of typhoid and dysentery, but also leishmaniasis, an exceptionally nasty skin disease which, left untreated, leads to permanent facial scarring. Before the war there were fewer than 3,000 cases in Syria, and there were some 250 treatment centers across the country. Now, as the sandflies responsible for spreading this condition breed out of control, as the trash piles up and sewage lines the streets, and with the treatment centers long shut down, there are estimated to be more than 100,000 cases, and counting.
Syria used to have free public hospitals and manufactured all its own medications. There were all kinds of specialists and allied health services, and medications were both accessible and affordable. Cheap, even: a month’s supply of anti-hypertensive cost about $1 (now, if you can get it, it’s 15 times that). Before the war, virtually everyone had running water and rubbish collection.
No vaccination means outbreaks of measles, and no pharmacies mean people dying of hypertension and heart disease. Food insecurity leads to malnutrition, rickets and increased vulnerability to infectious diseases. No contraception and no maternal health care lead to unplanned pregnancies at a time when antenatal and maternal health is denied. Without specialist surgeons, lacerations become loss of function, wounds become amputations.
If we can’t stop the killing in Syria, let’s at least pry open the borders so that aid and medical care will flow freely into Syria, instead of refugees flowing out, and we might at least curtail the spiraling of Syria from a middle-income country into a developing country with the diseases of poverty. And as the world mobilizes to stop the Syrian military’s use of chemical weapons, let us also mobilize to stop its use of another weapon of mass destruction: the deliberate attacks on medical care.
As a pediatric intensivist, general practitioner, public-health specialist, human-rights researcher and aid worker, I have worked in enough dodgy places over the last two decades to have seen a broad range of ill health and inhumanity. I am fully aware that hospitals were targeted in Bosnia, doctors were targeted in Cambodia, and aid workers have been targeted all over the world. But I have never encountered the scale upon which medical neutrality is being violated in Syria. This targeting of medical care has effectively become a weapon of mass destruction.
Annie Sparrow, a critical-care pediatrician and public health professional, is assistant professor of global health and deputy director of the human rights program at Icahn School of Medicine. This article was originally published on SyriaDeeply.com. To sign-up for SyriaDeeply's daily newsletter, visit SyriaDeeply.com.